Visual Inspection with Acetic Acid and Camera, or VIAC, is an effective way to prevent cervical cancer in women age 30-50 years old. It involves examining the opening of the womb, or the cervix, for changes that might lead to cancer. If these changes are detected early, the cells can be eliminated before they become cancerous. The cells are usually removed using a method called cryotherapy, or another method called LEEP. Both treatments are briefly described below.
VIAC examinations can also reveal possible advanced cervical cancer and certain noncancerous conditions such as chronic cervitis, pelvic inflammatory disease, and cervical polyps.
Visual inspection with acetic acid and treatment using cryotherapy or LEEP has been well-studied and is endorsed by the World Health Organization. WHO recommends using this “screen-and-treat” approach as an effective, low-cost way to reduce the incidence of cervical cancer in low-income countries. The disease is caused by the human papillomavirus (HPV), and it is the leading cancer killer of women in Zimbabwe and other sub-Saharan African countries.
The Zimbabwe Ministry of Health and Child Care has an established cervical cancer prevention program that offers VIAC screening and treatment at several of the nation’s major hospitals.
The VIAC procedure
- VIAC begins by swabbing the cervix with a vinegar-like solution of dilute acetic acid.
- If precancerous cells are present, the vinegar-like solution turns the abnormal cells white. This portion of the exam is the VIA—”visual inspection with acetic acid”—in VIAC.
- Next, a camera with a special lens is used to photograph the cervix. The photo helps identify the presence of abnormal, precancerous cells.
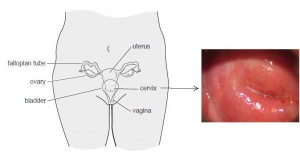
Figure 1. Left, the location of the cervix in the body. Right, a photo of a healthy cervix taken during a VIAC examination at St. Albert’s Mission Hospital.
Cervical cancer arises in the transformation zone of the cervix
The opening of the cervix is a place where two different types of cells meet. The cells that line the cervical canal (the “endocervix”) are tall, narrow, columnar epithelial cells. The cells that cover the surface of the cervix (the “ectocervix”), on the other hand, are squamous epithelial cells, which are very flat.
The place where the columnar cells meet the squamous epithelium is called the transformation zone. Cell division occurs at this junction, and it is in this junction that cervical cancer
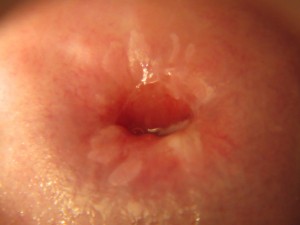
Figure 2. This photo of a cervix taken during a VIAC examination at St. Albert’s shows the white patches formed by precancerous cells.
occurs. Abnormal cells can arise here spontaneously or they can be induced by exposure to carcinogens such as certain strains of hPV or the chemicals produced during tobacco use. If these abnormal cells are not cleared by the immune system, they can progress to cervical cancer.
Why precancerous cells appear white after swabbing with dilute acetic acid
When precancerous cells arise, they have particular characteristics. They have larger nuclei and less cytoplasm, which is evidence of increased cell division (i.e., mitosis). When the cervix is swabbed with dilute acetic acid, the acid denatures the proteins in the precancerous cells, causing them to clump. It also dehydrates the cells. Light cannot penetrate these dense cells and instead is reflected back, making the cells appear white.
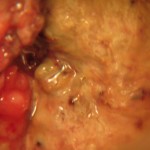
Figure 3. Photo taken during a VIAC examination at St. Albert’s showing a cervix with suspected cervical cancer. A definite diagnosis of cervical cancer requires further study of the tissue.
A nurse trained in VIAC can perform the screening exam, but if the exam reveals precancerous changes, possible cancer, or an inconclusive finding, the patient must be seen by a doctor for further care. If the precancerous cells are detected early enough, they are removed using either cryotherapy or LEEP, depending on their extent.
Cervical cancer develops over many years, passing through several stages. The earliest of these is the period in which abnormal cells are present but not yet cancerous. This precancerous stage is called cervical intraepithelial neoplasia (CIN). It is divided into three parts according to the degree of change present in the abnormal cells: CIN 1, CIN 2, and CIN3.
- CIN 1: The cells are mildly abnormal; they are not treated because they often clear up when left alone;
- CIN 2: The cells are moderately altered;
- CIN 3: The cells show a severe degree of change.
Women identified through VIAC screening as having CIN 2 and CIN 3 stage precancer should receive treatment, usually using cryotherapy or LEEP.
Cryotherapy
Cryotherapy, also called cryocautery, destroys precancerous cells by freezing them with ice-cold gas. It is used when the acetic-acid-induced white areas cover less than 75% of the ectocervix and do not extend into the endocervix. It is a simple outpatient procedure, and clients can go home the same day.
Note: After cryotherapy, a disharge from the vagina might continue for two to four weeks. It is generally a mild discharge and does not need treatment. But if it persists, the woman should see a doctor and a vaginal swab taken for culturing.
LEEP (Loop Electrical Excision Procedure)
LEEP removes abnormal areas from the cervix using a thin heated electrical wire that is passed through transformation zone. It is done under local anesthetic on outpatient basis. The affected tissue is sent for histological review. The margin of the excision is coagulated during the procedure, resulting in minimal bleeding. LEEP is used when the white areas cover more than 75% of the transformation zone or extend into the endocervix.
Both treatments have a healing period of two to four weeks, with certain restrictions on a woman’s activity during that time. Complete healing generally takes about a month.
A few women might experience after-effects that must be treated at a health facility. Following either procedure, a woman should return to the treatment location after about six weeks to be checked and to receive her laboratory report.
After any of these treatments
- Ask the doctor or nurse what to expect during the period of healing. Should you expect a discharge and how long will it last?
- What activities is it OK for you do and what activities should you avoid?
- What signs should you watch for that tell you you should return to the doctor?

if one is experiencing pains three months after leep what should she do
Dear Florence – LEEP (Loop Electrosurgical Excision Procedure) is one of the methods used to remove precancerous tissue from the cervix using a thin, heated wire. The procedure is done under local anesthesia. These symptoms may occur after LEEP, but they should disappear within two to four weeks: Watery vaginal discharge, pain of the type that is felt during a woman’s monthly period, and a little bleeding but not as much as is experienced during monthly period. NOTE: This information comes from the pamphlet “Post LEEP Client Instructions,” published by Zimbabwe’s Ministry of Health and Child Welfare.
If you are experiencing pain three months after your LEEP procedure, you should see a doctor as soon as you can to learn the cause.
I hope you can do so soon…Darrell
Is it safe to do viac while in the early stages of pregnancy like 3weeks since the procedure involves touching womb opening?
Dear Angeline – I forwarded your question to Dr. Paul Thistle, the obstetrician and gynaecologist at Karanda Mission Hospital. Here is his reply:
“VIAC should not routinely be performed during pregnancy because pregnancy causes physiological changes of the cervix that may interfere with the interpretation of VIAC results. That being said, VIAC is safe if performed in pregnancy. We encourage all women who suspect they are pregnant to seek early antenatal care, which includes a gynaecological examination. This examination would not include VIAC.”
I hope this answers your question, Angeline.
Keep well…Darrell
Is the procedure painful like the pap smear
Does VIAC also help detect cancer of the vulva or it’s just for cervical cancer
Hello and thank you for your question. VIAC screening is designed to detect changes on the cervix that can lead to cancer, but VIAC screening includes a thorough examination of the vulva, vagina and cervix. This exam may diagnose other conditions, such as cancer of the vulva, and noncancerous conditions such as polyps, discharge, warts, and other problems.
…Darrell
Thank you for writing. A VIAC exam should not be painful. Please consider writing again after your VIAC screening and describe your experience.
Thanks…Darrell
can e viac be compromised by menstrual cycle that’s approaching
Hello and thank you for your question. A VIAC examination requires a clear view of the cervix, so a woman should obtain her screening exam before menstrual bleeding begins or after it has stopped and has cleared up. I hope this is helpful. Thank you and keep well…Darrell
Hie . I live Overseas and have been having pap smears . Some are saying VIAC is the modern way of checking for cancer. I went to my doctor requesting for a VIAC and she stated that they dont do it here its outdated. Please help. Am confused now. Thanks. Patience
Hello, Patience, and thank you for your question. You have no cause for worry. Pap testing, also called “cytology,” is a highly effective test that is used to screen women for early signs of cervical cancer. It is the oldest screening test used to prevent cervical cancer. The test involves gently scraping the cervix to collect a sample of cells. The sample is placed on a microscope slide and specially stained to reveal the cells. That preparation is called a Pap smear. A doctor (that is, a pathologist) examines the cells in the sample using under a microscope. He or she looks for abnormal cells that show signs of being pre-cancerous or cancerous. Pap testing usually requires a woman to return to the doctor to repeat the test over a number years to monitor her for the appearance of pre-cancerous cells.
In addition to the Pap test, two other methods are used to screen women and prevent cervical cancer. One of these is VIAC, which stands for visual inspection with acetic acid and cervicography (photographing the cervix as part of the test for quality control). VIAC reveals the presence of abnormal cells that might be precancerous. The presence of those cells is revealed immediately, and the woman can be treated during the same visit using cryotherapy or another therapy that destroys the abnormal cells. VIAC is a relatively inexpensive and effective method for preventing cervical cancer. Unlike Pap testing, it usually does not require the preparation microscope slides that must be examined by a pathologist. (However, when a VIAC exam suggests that cancer might be present on the cervix, a biopsy of the abnormal cervical cells will be taken and the sample sent to a pathologist to confirm that cancer is present.)
VIAC is therefore a relatively inexpensive screening method, compared to Pap testing, and screening and treatment are possible during one visit to the clinic, making it more convenient for women who must travel long distances and have little or no money. Studies have shown that VIAC does prevent cervical cancer, and the method is endorsed by the World Health Organization for preventing cervical cancer in under-resourced countries. But VIAC is less precise than Pap testing. Abnormal cells that are revealed by VIAC might not truly be pre-cancerous; they might be abnormal of other reasons. However, the incidence of cervical cancer is very high in Zimbabwe and the region, in part because of the high rate of HIV infection, so treating all abnormal cells revealed by VIAC as pre-cancer can save many lives of women, keep families together and prevent children from becoming orphans.
The third and newest method of preventing cervical cancer is to test women for the presence of HPV infection. HPV, the human papillomavirus, causes nearly all cases of cervical cancer. If a woman is not infected with HPV, she is unlikely to develop cervical cancer. Unfortunately, HPV testing remains too expensive for most under-resourced countries, but we hope it will one day be available worldwide. (Use of HPV vaccination can also protect girls, boys, women and men from HPV infection to start with and thereby prevent cervical cancer.)
Thanks, Patience, and keep well…Darrell
Thanks Darrell . I recently had the HPV testing. All good.
That is great news, Patience. Thank you for writing back.
Keep well…Darrell
hie what are the effects of having sex a week after cryo
Hello, Kim, and thank you for your question. Zimbabwe Ministry of Health and Child Welfare guidelines say that a woman should not have sexual intercourse for one month after cryotherapy so as to avoid infection while the cervix is healing.
Keep well…Darrell
hello doctor when a cervix is diagnosed as clinically suspicious ,who long can one wait before the colonoscopy.what are the effects of delay?
Hello, and thank you for your question. I am not a doctor, but I have forwarded your question to a doctor in Zimbabwe. I will add his reply here after I receive it. In the meantime, I will say that when abnormal cells on the cervix are classified as suspicious of cancer, a sample of your cells — a biopsy — would have been taken and sent to a pathology lab. There a specialist will examine them under a microscope and confirm whether or not they are cancer cells. If the pathologist confirms that they are cancer cells, your doctor, nurse or midwife at the VIAC clinic will tell you and refer you to a clinic that specializes in treating cancer patients. You should try to learn whether your cells were cancerous or not as soon as possible and seek treatment as soon as possible. Thank you and I hope all goes well for you…Darrell
hie please help my wife recently had a vaginal discharge with a bad odour and when we went for some STI tests there were no signs of STI but when seeking medication the nurse wrote that it was an STI, we are now confused coz the tests revealed that we had none
Dear Sir – Thank you for your email. It is important to learn whether or not your wife has an STI and to learn what is causing her vaginal discharge. I am not a doctor, but I checked with Dr. Julia Musariri at St Albert’s Mission Hospital in Centenary about your problem. Dr. Musariri recommends that your wife have VIAC screening done, if she has not already done so. She should also tell them about the vaginal discharge and odour. Dr Musariri also recommends that your wife have a blood test, a test for urine sugar and perhaps have a vaginal swab taken for microscopy and culture. She should probably also begin taking the medication that was prescribed. I hope your wife can see a doctor soon and that her problem is quickly corrected. Best regards…Darrell
hi
Is there any danger to a growing fetus if you get the test done in early trimester pregnancy
Nice information
Which Western country is using this method and to what extent. I ask because people in Africa have become reluctant to use someone these new technologies because there is growing anxiety among us emanating from rumours that we are being used as medical guinea pigs. Statistics and background of this procedure would be helpful to help us make decisions
Answer to Precious:
Hello Precious
Your question raises an important concern about whether Africans are being used as experimental subjects in the visual inspection with acetic acid and cinematography (VIAC) program. Actually, VIAC is an established method of detecting cervical cancer and also pre-cancerous changes in the cervix. The principle is based upon the fact that a dilute (weak) solution of acetic acid (vinegar) is painted on to a cervix. If there are pre-malignant or malignant cells present in the cervix, the affected area will turn white. With the area of concern being identified it can easily and safely be removed by freezing it, or using electrocautery (a way of destroying the cells by heating them, that is safe and effective and quite simple to do).
The VIAC technique is encouraged by the Ministry of Health of Zimbabwe as a cost-effective means of distributing screening for this lethal cancer throughout the nation. Unfortunately, the challenging economic environment in Zimbabwe has made it difficult for the government to hire the necessary personnel and equipment to penetrate the entire nation. In our program we are collaborating with physicians and nurses at the Karanda and St. Albert’s Mission Hospitals and have external grant support to cover the program’s costs.
To be sure, this is not experimental and it has been enthusiastically embraced by thousands of Zimbabwean women since we started.
Thank you for your inquiry.
Hello Precious
Your question raises an important concern about whether Africans are being used as experimental subjects in the visual inspection with acetic acid and cinematography (VIAC) program. Actually, VIAC is an established method of detecting cervical cancer and also pre-cancerous changes in the cervix. The principle is based upon the fact that a dilute (weak) solution of acetic acid (vinegar) is painted on to a cervix. If there are pre-malignant or malignant cells present in the cervix, the affected area will turn white. With the area of concern being identified it can easily and safely be removed by freezing it, or using electrocautery (a way of destroying the cells by heating them, that is safe and effective and quite simple to do).
The VIAC technique is encouraged by the Ministry of Health of Zimbabwe as a cost-effective means of distributing screening for this lethal cancer throughout the nation. Unfortunately, the challenging economic environment in Zimbabwe has made it difficult for the government to hire the necessary personnel and equipment to penetrate the entire nation. In our program we are collaborating with physicians and nurses at the Karanda and St. Albert’s Mission Hospitals and have external grant support to cover the program’s costs.
To be sure, this is not an experimental procedure, and it has been enthusiastically embraced by thousands of Zimbabwean women since we started.
Thank you for your inquiry.
Dr. Lowell Schnipper
After VIAC, white cells were detected. Does that mean you have cancer? If booked for leep two months from now, is one safe?
Hello Gamuchirai and thank you for your question. To answer your question, I checked with Dr. Paul Thistle, the obstetrician/gynaecologist at Karanda Mission Hospital, and with oncologist Dr. Lowell Schnipper. A VIAC-test finding of white cells on the cervix does NOT mean you have cancer. VIAC detects cells on the cervix that are abnormal and that might or might not become cancerous with time. To sure and to prevent cervical cancer from developing, the abnormal cells should be removed. Sometimes they are removed using LEEP and sometimes they are removed using cryotherapy.
Regarding your appointment in two months for LEEP, it takes time for abnormal cells to evolve into early stage cervical cancer. Your time period of two months should be fine.
Thanks again and keep well…Darrell
I want to see a specialist in zimbabwe.i bleed after sex and i have brown like discharge.is there any doctor in bulawayo
Hello, Charity. Yes, you can talk to a specialist, an obstetrician/gynaecologist, in Bulawayo at UBH Lady Rowell Maternity Hospital, or Mpilo Hospital or Mater Day (Dei) Hospital.
I hope this helps and that all goes well for you.
…Darrell
Hello,
Please may I kindly inquire – where exactly is VIAC screening taking place in Zimbabwe? Would you by any chance have a list of the hospitals/clinics/centers or know who I could reach out to for this information?
Thank you for your assistance in advance.
Kind Regards,
Thembie.
Hie Darrel. What are the side effects of VIAC tests. Is it normal to have watery discharge after the examination. I was normal before I was examined.
Hi, Spoonky – Thank you for your question. Normally there should be no discharge after VIAC testing. If it has continued, it would be good to talk to your doctor. Best regards, and I hope all goes well for you…Darrell
Is it normal to start having a very painful womb after a year i did VIAC?…Does that mean i should do another one please help
Worried
Hi, Josey – A woman should not be in pain after a normal VIAC exam, especially after a year. Please see your doctor as soon as possible to learn the cause of your pain. Thank you for writing and I hope all goes well for you.
…Darrell
Hi, Spoonky – Thank you for writing. There should be no serious side effects after a normal VIAC exam. Please return to the clinic or see a doctor to learn the cause of the watery discharge. Thanks and I hope all goes well for you. …Darrell
Hello, Thembie. I’m sorry for this delayed reply. VIAC screening should be available at national and provincial hospitals.
If you are nearer to Bulawayo, you can go to UBH, or Mpilo or Mater Day Hospital. In Harare, Pari should offer VIAC screening.
Because of the current economic conditions, it might be helpful to ask your female friends if they have had VIAC and where they went. Some clinics might be better equipped than others.
Further north, I know that VIAC screening is available at St. Albert’s Mission Hospital and Karanda Mission Hospital.
Thank you and I hope this is helpful…Darrell
Hie darell.i was diognised for cryotherapy and i went for cryotherapy done the following day.so my question is after hw long should i start to see those discharges after cryotherapy been done
Hello, Carol, and thank you for your question. I sent your question to Dr. Paul Thistle at Karada Mission Hospital. In answer to your question, Dr. Thistle replied: “The average length of discharge after a cryotherapy procedure will be 2 weeks. If the discharge persists for longer than one month you should consult your health care provider; you should see your provider sooner if you have persistent abdominal pain, bleeding, fever or chills.”
Thank you again, Carol. I hope all goes well for you. …Darrell
Hi, Kay – Thank you. Dr. Paul Thistle at Karanda Mission Hospital wrote to answer your question:
VIAC is usually recommended every three years in healthy women, with no previous abnormal screenings.
For women living with HIV, screening is recommended every year.
Do u offer yo services in SA and where
Do you feel any pain after VIAC? A test was done yesterday but I am feeling a pain down there
Hi ..What if you can feel lumps on the cervix opening can they go away on their own or VIAC IS NEEDED
does viac help on conception i heard some says after viac u can easily get pregnant how true is it
Hie is it normal to have pain when urinating 2 days after doing VIAC and the results were negative
Thank you for your question. I am not a doctor, but I checked with Dr. Paul Thistle at Karanda Mission Hospital. Here is his reply:
“This lady may have a concurrent infection, such as a urinary tract infection. She should see her doctor for further assessment and possible treatment.”
I hope this is helpful.
…Darrell